31 Mar 2026
Nicola Menzies-Gow MA, VetMB, CertEM(IntMed), DipECEIM, FRCVS discusses why so many domesticated equines are overweight, and what can be done to manage this common problem.

Image: Jelena / Adobe Stock
Obesity is defined as the accumulation of adipose tissue to the extent that it has a negative impact on health, leading to reduced life expectancy and/or increased health problems.
Obesity is increasingly common and has significant detrimental effects on the health of horses and ponies, similar to the human and companion animal population. While 26% of pet cats and 25% of pet dogs are overweight, UK studies report that around 50% of horses and ponies are fat or very fat1, with rates in some populations of native ponies being as high as 70%2.
Obesity is also more common in animals described as good doers, animals used for pleasure or non-ridden, and show or dressage animals2, as well as in summer compared to the end of winter3. In addition, owners consistently underestimate the level of obesity of their animal4, and the perception of ideal weight for show and dressage animals is greater than for other disciplines, as fat is misconstrued as muscle. Therefore, veterinarians need to be proactive in identifying overweight horses and educating clients about the associated health risks and management of the overweight horse.
The reasons that domesticated animals develop obesity are similar to those attributed to obesity in humans, namely physical inactivity combined with the consumption of excessive calories. As an herbivorous species, horses have evolved to rely on poor-quality grass forage alone for their nutritional requirements. As a result, during the summer and autumn, horses should ingest increasing quantities of available forage and gain adiposity in preparation for the winter, when food tends to be scarce and weather conditions harsh.
Increased secretion of the hormone proopiomelanocortin by the pituitary pars intermedia during these seasons stimulates appetite and adipogenesis. These changes represent a critical survival mechanism that ensures that stored energy in the form of body fat is available throughout the winter months.
Normally, the period of food scarcity is finite and the acquired fat stores are depleted just prior to the onset of spring and resumption of grass growth. Therefore, in the wild, acquisition of adipose tissue in summer and autumn is essential for winter survival. The development of insulin dysregulation (ID) is a critical component of this winter survival mechanism, which seems to develop and resolve in parallel with the acquisition and depletion of additional fat stores at the start and finish of winter, respectively. Therefore, the horse is evolutionarily designed to be a yo-yo dieter.
The modern husbandry practices of providing excessive calories in the form of high-quality pasture and bucket feeds, physical inactivity, stabling and the use of rugs to help maintain body temperature year round all promote fat storage and/or decrease the use of stored fat, and consequently encourage the acquisition of excessive adiposity and its chronic persistence. This is further compounded by owners striving for their horses to look their “best” year round. The perception of “best” has morphed over time from horses that are well muscled for work or sport to horses that are instead well covered in fat. Many owners do not appreciate the difference between muscling and fat deposition, and the trend toward promoting increased fat deposition has been re-enforced by rewarding obesity in the show and dressage arenas, and by the frequent depiction of obese horses as role models on websites, in the equestrian press and elsewhere. Additionally, obesity is often trivialised, with obese animals depicted in cartoons, the use of endearing terms such as “cuddly”, “tubby” or “podgy”, and the lack of a social stigma associated with keeping an obese animal. By contrast, the sight of a thin or emaciated horse evokes horror and accusations of cruelty. The result is the persistence of obesity and, subsequently, ID year round.
Obesity has been shown to have several adverse systemic effects in horses including:
A number of health disorders are associated with equine obesity either directly due to the physical presence of the adipose tissue or indirectly due to associated ID (Table 1).
ID occurs in obese horses due to altered adipose tissue derived hormone (adipokine) production, including increased production of certain hormones that antagonise insulin (for example, leptin) and decreased production of certain hormones that sensitise to the action of insulin (for example, adiponectin).
Obesity is most accurately assessed at postmortem by carcase dissection or by administration of deuterium oxide9. However, in clinical practice, generalised obesity is assessed by body condition scoring (BCS)10 that can be performed using a 0 to 5 or 0 to 9 scale11. The latter is more robust, but seems to be used more frequently in the research setting. Either scale is acceptable, provided the denominator is stated as, for example, a BCS of 5 out of 5 is obese, whereas 5 out 9 is ideal body condition. Regional adiposity is assessed using cresty neck scoring (CNS; Figure 1).
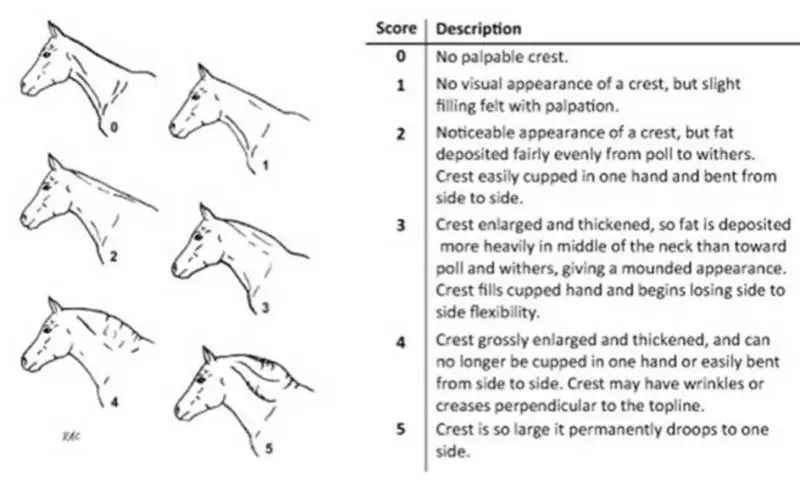
Ultrasonographic measurements of fat depth at specific anatomic locations can be used to assess adiposity, but have their limitations12,13. The assessment of retroperitoneal fat depth by ultrasonographic examination of the ventral midline may be useful in demonstrating horses that are thin on the outside but fat on the inside (so-called TOFIs).
Serum insulin and the adipose tissue-derived hormone adiponectin are independent risk factors for laminitis14, so measurement of both in overweight animals can be useful in persuading owners that their horse has metabolic disease and would benefit from a programme of weight loss. Measurements of insulin concentration at baseline or after a carbohydrate challenge (for example, oral sugar test) are useful in assessing laminitis risk14 and in monitoring improvement in insulin sensitivity in response to weight loss.
Obesity can be reduced through the implementation of a regime of dietary changes in conjunction with increased exercise in sound animals. An ideal target for weight loss is 0.5% to 1% of body mass (BM) weekly.
Overweight or obese animals should be fed a diet based on grass hay (or hay substitute) with low (less than 10%) NSC content, and cereals avoided. A daily allowance of 1.25% to 1.5% of actual BM as dry matter intake (DMI), or 1.4% 1.7% of actual BM as fed, is widely recommended. Soaking hay in water before feeding can be done to leach water-soluble carbohydrates, and ideally forage should be analysed after soaking. However, hay analysis is only practical if an owner has many bales from the same source. If this is not the case, and bales are bought a few at a time from multiple sources, then while soaking does not reliably decrease the NSC content to less than 10% in every case15, it will help. It should be remembered that steaming hay does not reduce NSC content.
Feeding haylage should generally be avoided, as haylage typically has a higher NSC content; is more palatable, so intakes may be higher; and seems to result in a greater insulin response than a comparable hay16. However, some haylage can have a low NSC content and, if fed in restricted quantities, may be suitable if it has been analysed. Barley straw can be fed to maintain appropriate levels of fibre and total intake while reducing calorie intake. A recent study demonstrated that horses fed a 50:50 hay:straw diet lost weight while those fed hay did not17.
The forage should be divided into as many feeds per day as practically possible and strategies employed to prolong feed intake time, such as use of haynets with small holes, double haynetting, haybags and haynets hung from the ceiling in the middle of the stable.
In most overweight animals, any access to pasture is going to severely frustrate attempts at weight loss, as intake cannot be accurately controlled. It is, therefore, best to remove the horse from pasture, at least initially. When an animal is subsequently turned out to pasture, although this will have the beneficial effect of increased exercise and allow social interaction, methods to restrict intake should be used such as strip grazing, track systems, restriction of turnout time, grass muzzles and keeping pasture height short through topping.
Forage-only diets – especially if the forage is soaked – do not provide adequate protein, minerals or vitamins, and so a low-calorie commercial ration balancer product that contains sources of high-quality protein and a mixture of vitamins and minerals to balance the low vitamin E, vitamin, copper, zinc, selenium and other minerals typically found in mature grass hays, is recommended.
Advice on feeding needs to be simple and specific for owners to be able to implement the changes in their daily life. For most owners, compliance will be improved if a specific “recipe” is provided which dictates exactly what quantity of exactly what feed (such as the trade name) is required. Providing general advice and telling owners that they need to feed 1.5% BM of a feed with less than 10% sugar is unlikely to result in good compliance, because it may be hard for them to put these figures into practice.
Instead, vets should be dispensing weight tapes and luggage scales for weighing forage, alongside a written feed plan that has been formulated together with the owner, so as to take into account what is actually possible. Owners should be reminded that the use of a single scoop for different feeds can result in overfeeding, as they measure volume rather than weight, with the weights of feeds varying considerably, and the scoop needs to be calibrated for each feed.
Finally, owners should be encouraged to weigh out the total amount of food for the day, before it is subsequently split into separate portions. Creating and weighing individual portions has been seen to lead to a tendency to feed at the top end, or even slightly over the recommended weight each time, and weighing once reduces the percentage error.
Unless a musculoskeletal reason exists for not doing so, animals should be exercised daily, as this has been shown to improve insulin sensitivity and decrease food intake, as well as consume calories. Exercise undertaken in any animal needs to have a gradual increase in the intensity and duration according to fitness level.
Recommendations around desired exercise levels are largely opinion based, yet to achieve compliance, any exercise programme needs to be both specific and realistic. In a recent consensus statement18, the following exercise recommendations were made:
Alternatively, a protocol for 50 minutes of exercise was proposed recently, with a 10-minute warm up at walk and then alternating trot sets and walk breaks of five minutes each, finishing with a five-minute cool down19. It was suggested that this protocol be performed five days per week. As horses become fitter, the trots sets can be replaced with canter.
Horses are able to thermoregulate at temperatures between 5°C and 25°C and, therefore, require no additional measures to control their body temperature, such as rugs between these temperatures. Horses that are acclimatised to lower temperatures are able to thermoregulate at temperatures as low as -10°C to -15°C. When hotter than 10°C, horses prefer not to be rugged except in extreme wet or windy weather conditions. Therefore, if the weather is neither wet nor windy, then rugs are only required at less than 5°C, and acclimatised horses may only require rugs below temperatures as low as -10°C.
Rugging horses in cold weather can effectively reduce energy demands by 18%, resulting in reduced calorie utilisation. Unnecessary rugging represents a welfare concern in causing horses to become too hot in warmer weather such that they are unable to thermoregulate, whereas depriving horses of rugs is less likely to impact on their welfare. Provision of a field shelter that provides protection from the wind and rain is a far better solution to cold weather than rugging. However, geriatric horses may be less able to thermoregulate at lower temperatures.
Pharmacologic agents should be considered for short-term use (three to six months) in animals that are weight loss resistant, cannot be exercised for lameness reasons or have acute laminitis and require more rapid weight loss than can be achieved with management changes alone.
Levothyroxine is the most appropriate pharmacologic treatment for promoting weight loss through speeding up the metabolic rate and has also been demonstrated to improve insulin sensitivity20. It is essential that compliance with the dietary recommendations takes place when using levothyroxine or weight loss is unlikely to result due to the side effect of polyphagia. No licensed product is available in the UK; therefore, levothyroxine can be prescribed under the cascade at a dose of 0.1mg/kg by mouth once daily for a period of three to six months or until the target for weight loss is achieved. When treatment is to be discontinued, it is recommended that the dose is halved for two weeks, then halved again for a further two weeks before treatment is stopped.
If the health risk is associated with ID, then use of a sodium glucose cotransporter-2 inhibitor (SGLT2i) can be considered. SGLT2i are a novel class of oral hypoglycaemic agents used in conjunction with lifestyle changes in the management of human metabolic syndrome and type 2 diabetes mellitus. No licensed veterinary drugs are available for treating ID and preventing insulin-associated laminitis in horses, but drugs that have been reportedly used in the horse to date include the gliflozins velagliflozin21, canagliflozin22, ertugliflozin23 and dapagliflozin24.
These drugs have been shown to improve insulin sensitivity, correct hyperglycaemia (if present) and improve laminitis pain in the majority of animals. Although this only holds true if diet control, exercise when possible and adequate treatment of pituitary pars intermedia dysfunction are maintained. If these drugs are used, then this should be done under strict veterinary supervision with monitoring of insulin sensitivity and triglyceride concentrations, as well as serum activities of hepatic enzymes due to the potential for deleterious side effects. It should also be remembered that these drugs will not improve insulin sensitivity in all animals.
Weight loss should be monitored every four to six weeks by the owner. Ideally, this should be done using a weigh bridge; however, this is not usually possible. Instead, the most reliable method involves heart and belly girth measurement or use of a weight tape, as these will decrease as body weight decreases.
In contrast, BCS will often remain unchanged for a prolonged period, as it is a non-linear scale, and marked weight loss will be required before the score will change, resulting in the owner becoming disheartened when no improvement is apparent. CNS is also less reliable, as the crest contains a large amount of fibrous tissue that will remain even with marked loss of adipose tissue.
It is important to find markers that provide owners with gratification, and heart and belly girth are, therefore, the most suitable. It is also important to consider regular veterinary check ins to ensure that the weight loss is going according to plan and allow any necessary adjustments to be made.
Targets are helpful and provide a sense of purpose, so it is useful to provide charts to monitor morphometric characteristics and bodyweight. Targets for exercise based on working towards the owner’s aspirations (for example, to get the horse fit enough to enter a sponsored ride or undertake a specific activity) are also a powerful motivator1. Use of apps that allow exercise targets to be set and progress to be tracked can also be helpful.
In horses with weight loss resistance, a further forage restriction to 1.0% BM as DMI or 1.15% BM as fed may be considered if appropriately monitored. However, it is preferable not to decrease forage provision to less than 1% of target bodyweight, as this may increase the risk for hindgut dysfunction, gastric ulcers, stereotypical behaviours, ingestion of bedding or coprophagy.
Once the target weight is achieved, it is important that monitoring of weight by the owner is continued, or experience from other species indicates that diet and management changes will not be maintained in a large proportion of cases, and many will return to an obese state.
Equines that have lost weight may still exhibit ID and, if they do, should continue to be fed low sugar/starch (less than 10% to 12% NSC) feeds that will limit the glycaemic and, therefore, insulinaemic response. A high-fibre, low-cereal diet will be healthier, so any return to feeding cereals after weight has been lost should be discouraged.
Any subsequent gain in weight, however transient, may be associated with decreased insulin sensitivity and, therefore, increased laminitis risk.
Nicola Menzies-Gow qualified from the University of Cambridge in 1997 and, after three years in first opinion equine practice in Essex, joined the RVC, where she completed a residency in equine medicine and a PhD. Now a senior lecturer in equine medicine, Nicola’s clinical interests focus on endocrinology, cardiology and general medicine.