10 Feb 2026
Karen Carver RVN and Ingrid Tundo DrMedVet, DipEVDC, MRCVS explain how to spot this common dental problem in dogs and help owners manage their oral health at home.

Figure 1. Periodontal anatomy.
Periodontal disease is one of the most common dental conditions affecting dogs; yet, it often goes unnoticed due to its slow progression, patient resilience and the subtle nature of its early symptoms.
This condition, which affects the structures surrounding the teeth – which include the gingiva, cementum, periodontal ligament and alveolar bone – can lead to pain, infection and, ultimately, tooth loss, if not addressed early.
Periodontal disease can have a significant impact not only on a dog’s oral health, but also on its overall well-being. Fortunately, periodontal disease can be managed and even prevented with early identification and diligent home care.
This article explores how to identify periodontal disease in dogs, the stages of the disease and how dog owners can effectively manage their pets’ oral health at home.
Periodontal disease refers to the inflammation and breakdown of the structures around the teeth.
It starts as gingivitis (inflammation of the gingiva) and, if left untreated, progresses to the deterioration of the periodontal ligament and alveolar bone that support the teeth (Figure 1).
Canine periodontal disease is classified into four stages based on the severity of the condition.
Gingivitis is the mildest form of periodontal disease (Figure 2). At this stage, the gingiva becomes inflamed. Plaque forms at the gingival margin, but the attachments and surrounding bone are unaffected.
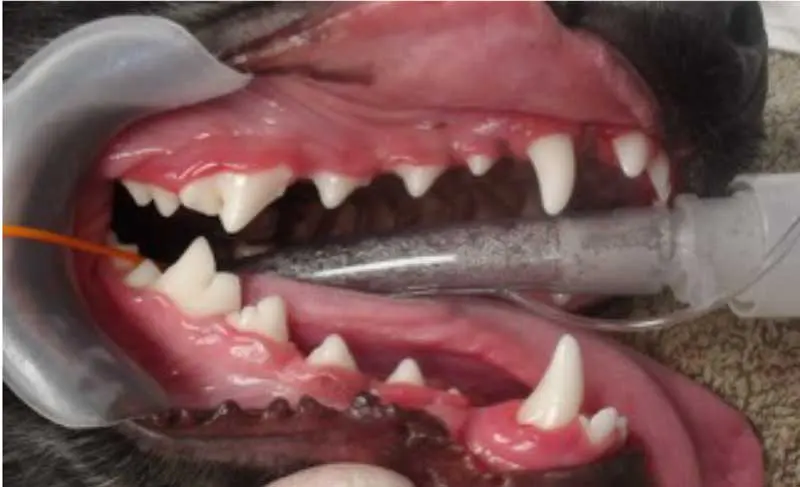
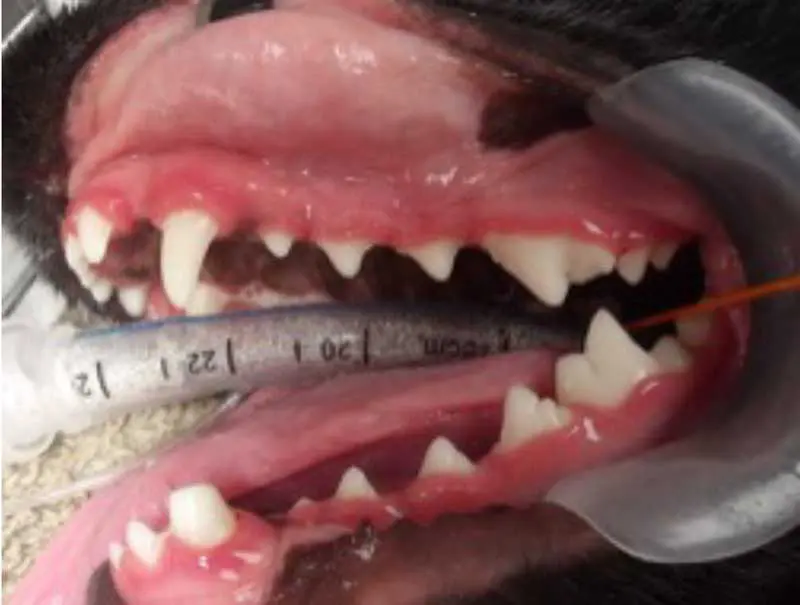
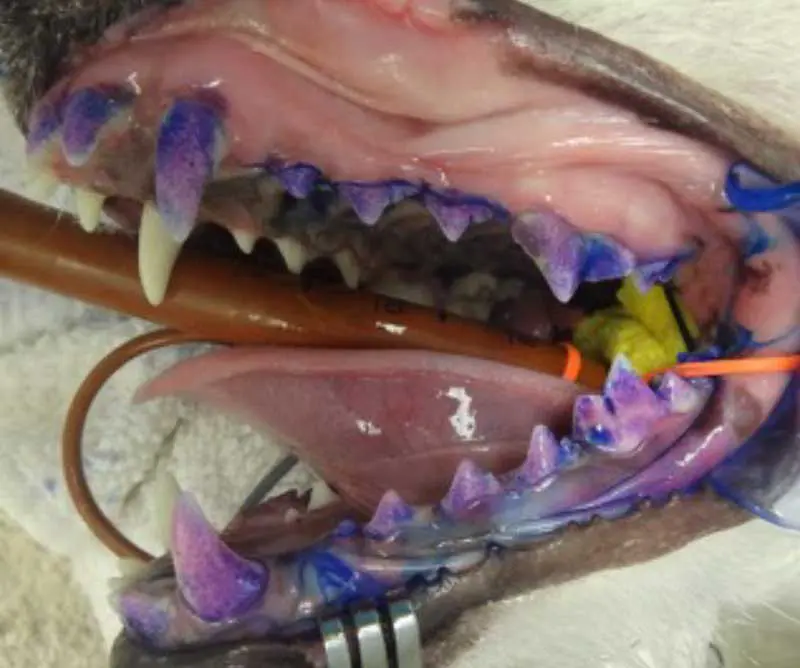
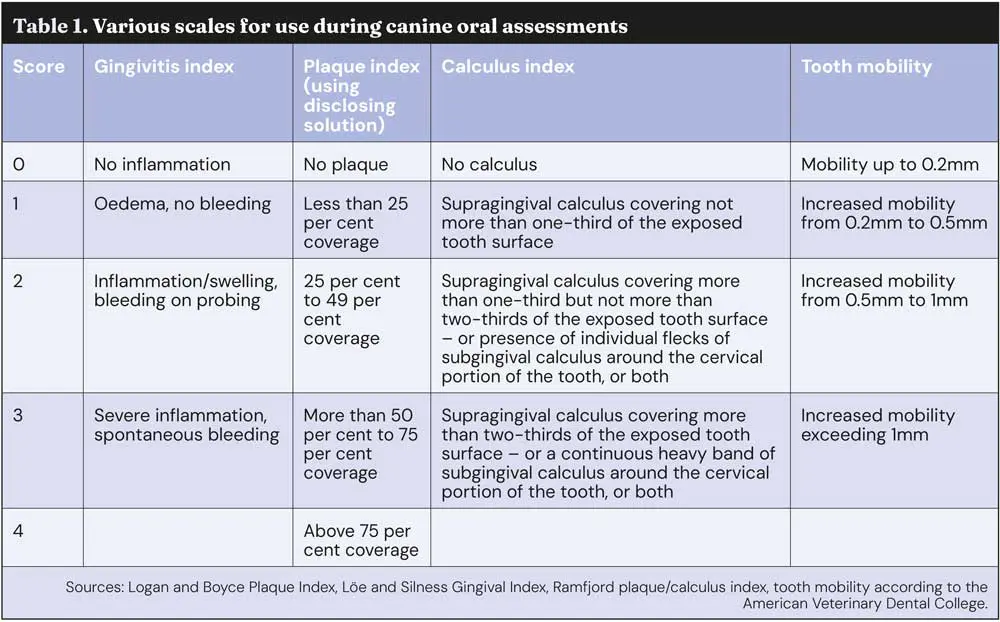
Remember that plaque is not always visible to the naked eye, so applying a plaque-disclosing solution can help highlight any areas which may be of concern (Figure 3). Gingivitis is usually reversible with appropriate home care, and symptoms may include:
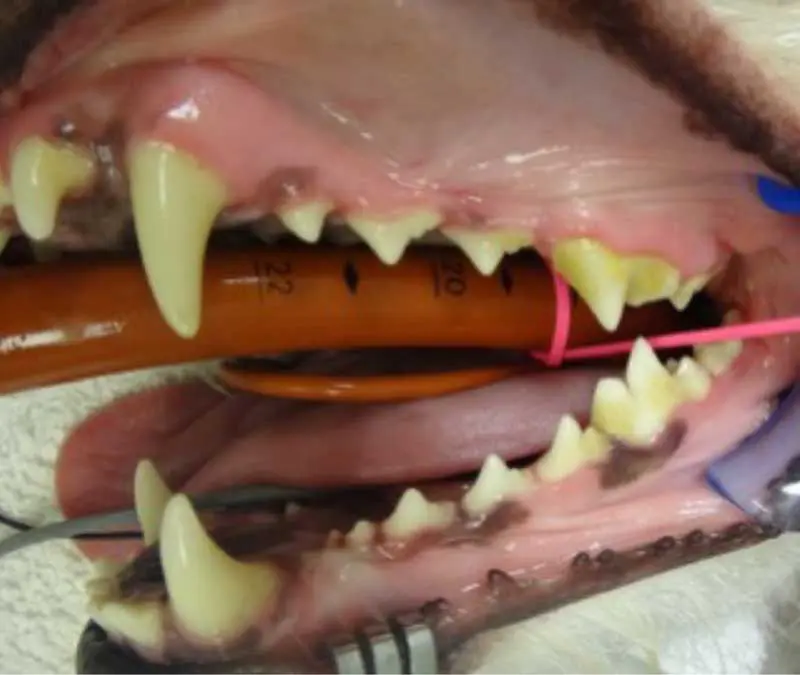
At stage 2, the inflammation extends below the gum line, affecting the supporting structures of the teeth (Figure 4). Osteolysis can be radiographically noticeable, with up to 25% bone loss.
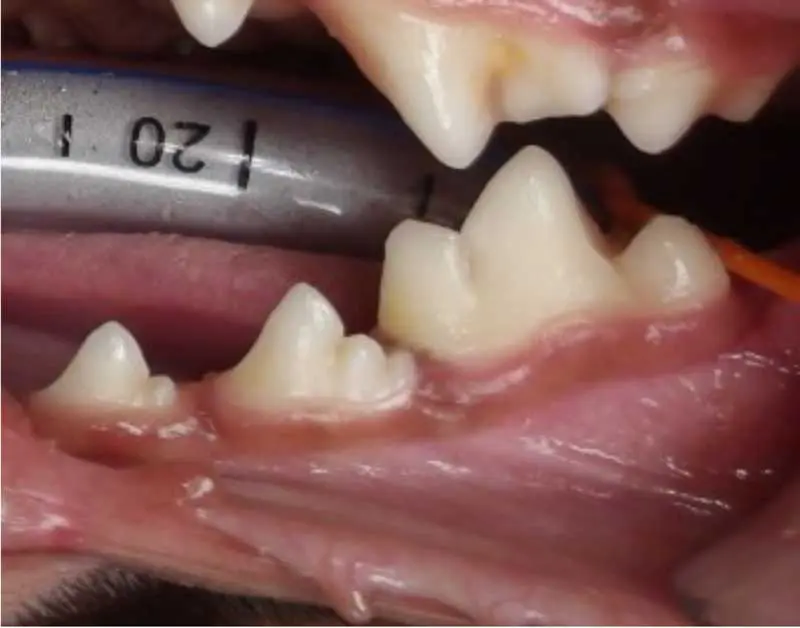
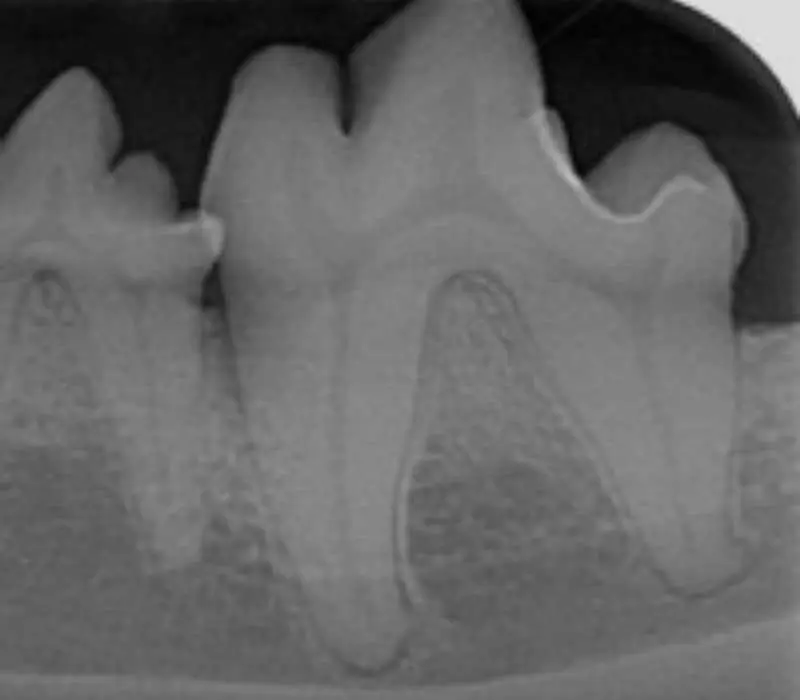
Symptoms of early periodontitis may include:
The attachment loss continues to progress, with 25% to 50% bone loss. Periodontal pockets form between the teeth and gingiva, and furcation of the teeth becomes exposed, harbouring bacteria and leading to further damage (Figure 5).
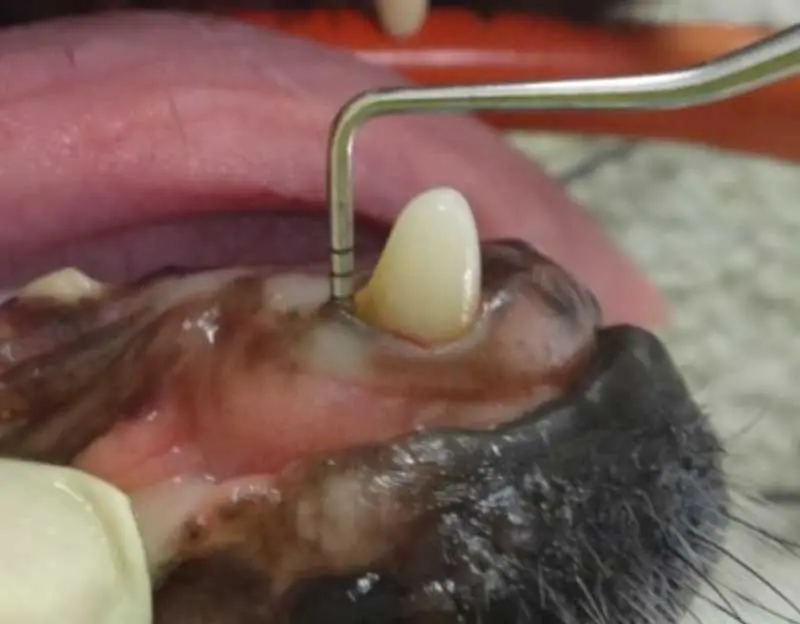
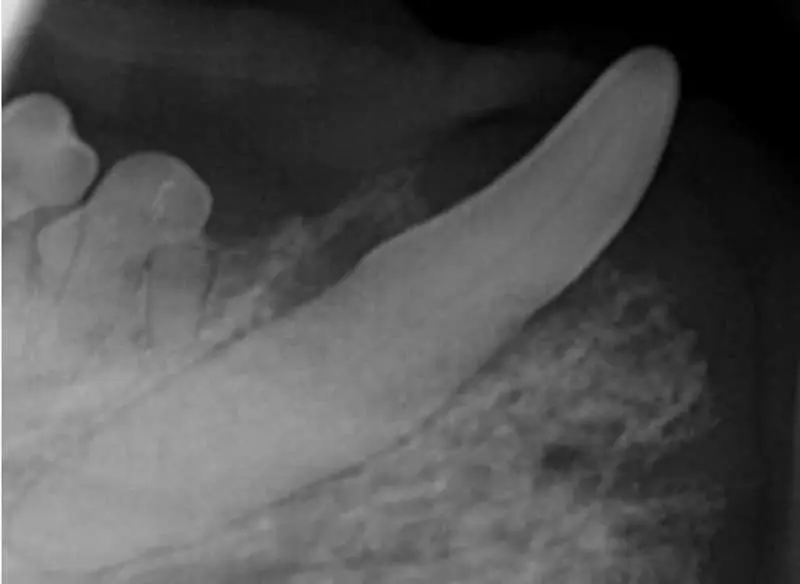
Symptoms may become more pronounced, including:
In the advanced stage of periodontal disease, bone loss exceeds 50%. At this point, tooth loss is common due to the loss of the alveolar bone and periodontal ligament. The patient may experience significant pain and discomfort (Figure 6).
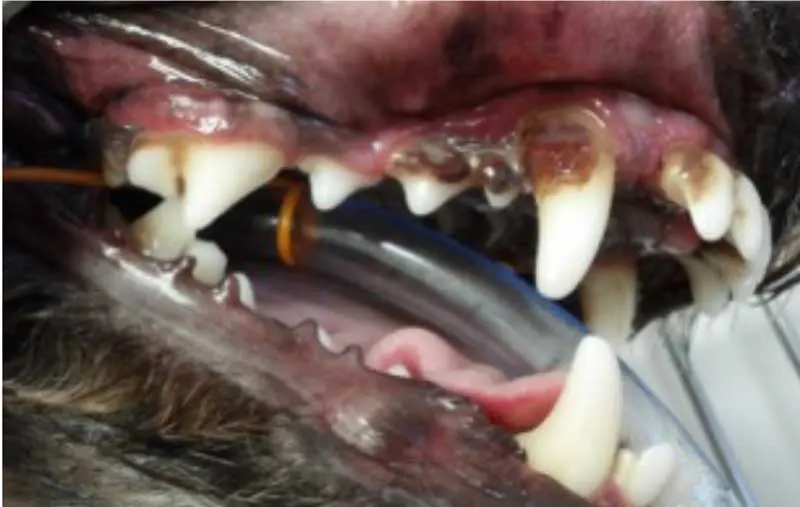
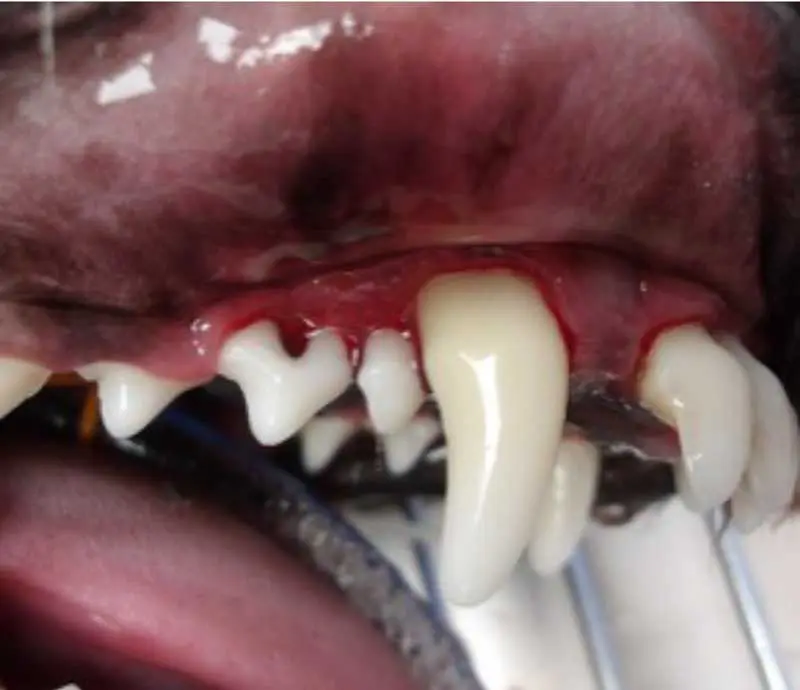
Symptoms may include:
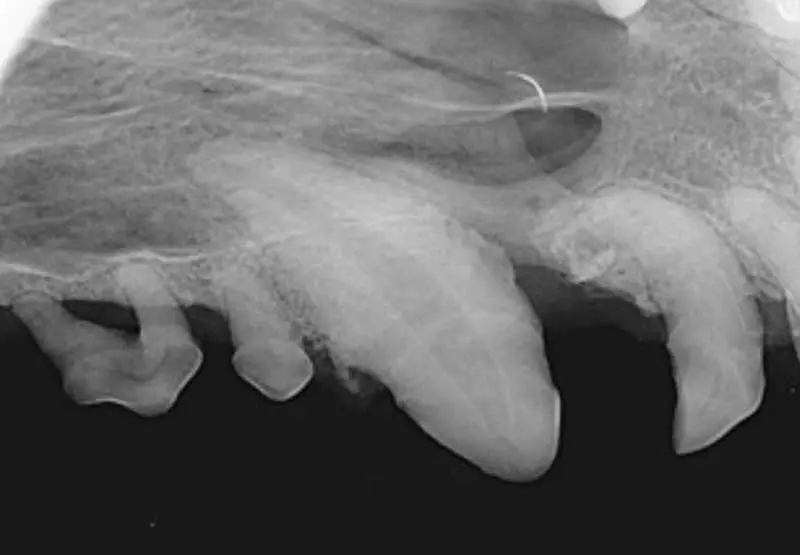
Crucial when dealing with patients with periodontal disease because it allows for a more empathetic approach to both the dog’s physical and emotional well-being.
Regional anaesthetic agents are commonly used in human and veterinary dentistry. They bind to sodium channels, blocking the noxious stimuli signals sent to the brain. This allows the veterinarian to remove discomfort during surgical procedures and promote a painless recovery.
The anaesthetic agents commonly used are lidocaine, bupivacaine and mepivacaine (Table 2).
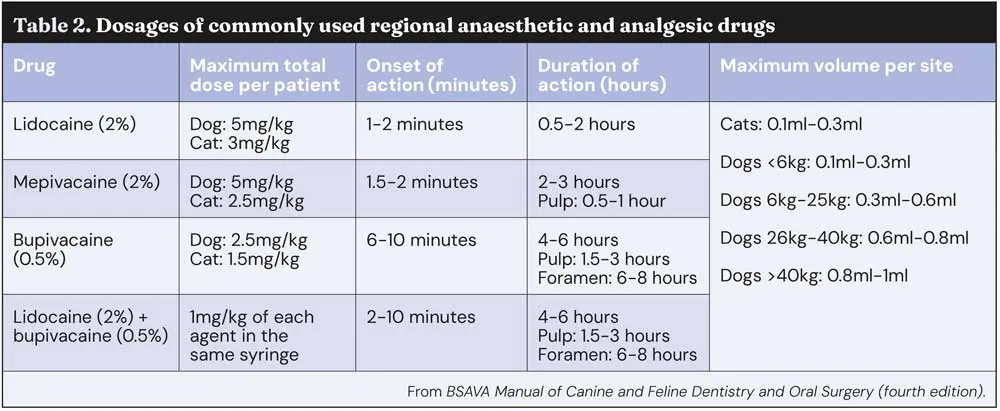
Studies have shown that analgesia resulted in a 23% reduction in isoflurane minimum alveolar concentration in dogs.
The most common local nerve blocks performed in veterinary dentistry are:
Several factors increase the risk of periodontal disease of dogs. These include the following.
Breed. Smaller dog breeds, such as the pug, dachshund, toy poodle and Yorkshire terrier, are more prone to dental problems due to their smaller mouths and crowded/rotated dentition.
Age. Older dogs are more likely to develop periodontal disease, as the build up of plaque and tartar increases over time if not dealt with.
Genetics. Some dogs are genetically predisposed to dental disease, which may lead to early onset of periodontal disease.
Poor oral hygiene. Inadequate home care significantly increases the risk of periodontal disease.
Underlying health conditions. Conditions such as autoimmune disorders may increase the likelihood of periodontal disease.
Periodontal disease can have serious consequences both locally in the oral cavity and systemically in the body.
Infection. Periodontal disease can lead to an infection in the oral cavity, which can worsen over time and spread deeper into the supporting structures of the teeth, including the bone, causing osteomyelitis.
Pain. As the infection progresses, it can lead to inflammation and sensitivity in the soft tissues, teeth, and alveolar bone. This can make chewing painful, cause discomfort when brushing, and sometimes lead to abscess formation, which results in localised pain.
Loss of function. Loss of periodontal support can cause the teeth to become mobile, making normal chewing or playing difficult and uncomfortable. Patients may result in chewing only on one side.
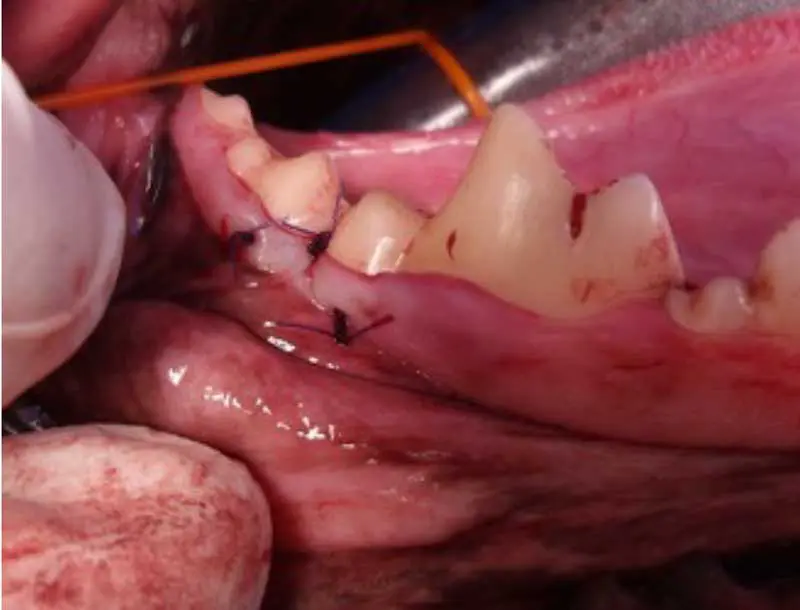
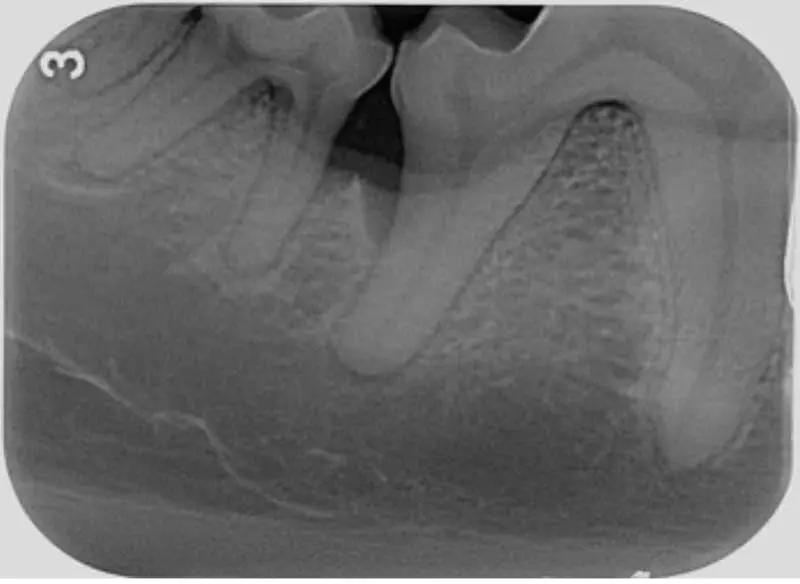
Loss of teeth and mandibular fractures. In severe cases, if left over time, the weakened bone structure may make the mandible more susceptible to pathological fractures (Figure 9).
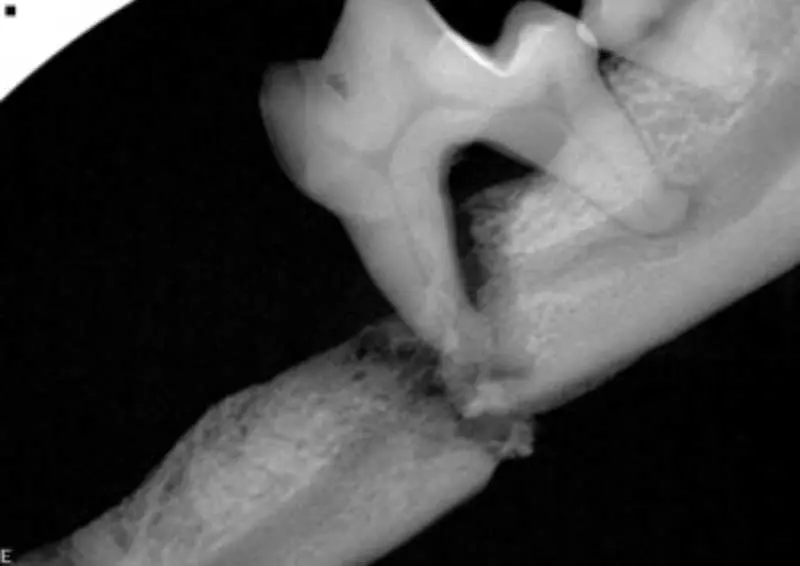
It has been proven in human medicine that periodontal disease causes systemic consequences. However, in veterinary medicine, wide-based studies have yet to be conducted to support this.
Inflammatory mediators’ effect. The inflammatory response triggered by periodontal disease is not confined to the oral cavity. The body releases inflammatory mediators, such as cytokines, which can enter the bloodstream and affect various organs. This systemic inflammation can contribute to the development of other chronic conditions, such as cardiovascular disease, and worsen existing conditions.
Bacteraemia. Periodontal disease can lead to bacteria from infected tissues entering the bloodstream, a condition known as bacteraemia. This is particularly concerning because the bacteria can spread to other parts of the body, potentially leading to infections in vital organs such as the kidneys, liver and heart.
Endocarditis. One of the most significant risks of bacteraemia is the development of endocarditis, an infection of the inner lining of the heart, often involving the heart valves, which can be life threatening.
Liver and kidney disease. Chronic inflammation and spreading bacteria from the mouth can impact the liver and kidneys. Persistent inflammation may stress the liver, and kidney function may be compromised. Human studies have linked periodontal disease to a higher risk of chronic kidney disease, and it may exacerbate conditions like liver cirrhosis.
Overall impact. Periodontal disease is not just a local oral health issue; it can have wide-reaching effects on a patient’s general health. Preventing and treating periodontal disease is crucial for maintaining both oral and systemic health. Regular dental check ups, good oral hygiene and managing risk factors such as underlying health conditions are essential to reduce these risks.
While professional oral assessment and surgical intervention are crucial for managing advanced periodontal disease, at-home care plays a vital role in preventing and managing the early stages of the disease.
Daily brushing remains the gold standard for maintaining oral health in dogs, and at least three times a week is the minimum, but daily is the best way to maintain good oral hygiene (Figure 10).

Using a soft toothbrush in small circular motions with toothpaste specifically designed for dogs is essential. Human toothpaste contains fluoride and other ingredients that are toxic to dogs.
Key points to remember include:
Dental toys and chews are an excellent way to help maintain a dog’s oral hygiene.
These products are designed to reduce plaque and tartar buildup as the dog chews on them. Look for products that have been approved by the Veterinary Oral Health Council, as they have been tested for efficacy. Be sure to select chews that are appropriate for your patient’s size and chewing habits. Some chews can be hard enough to damage teeth, so follow the “rule of thumb” and do not give patients toys you cannot pit with your thumbnail.
Some pet food brands offer dental diets that are formulated to promote oral health.
These foods contain larger kibble sizes that help scrape the teeth as the dog chews, and some are designed to reduce plaque build up.
Powdered food additives are available, which studies have suggested can inhibit plaque and tartar formation. The powder is a natural product and is sprinkled on to the patient’s food daily.
Water additives that can help control bacteria and reduce plaque formation are also available. These additives are mixed into a patient’s water and can be a convenient way to support oral health, but they are not a replacement for brushing.
Routine veterinary check ups are essential for identifying early signs of periodontal disease and preventing further damage.
A conscious oral assessment is something that can be performed at any check up (patient-dependent). Registered veterinary nurses can set up dental clinics in their practices to allow an optimum time frame to discuss oral hygiene and prevention with clients.
Oral assessment under general anaesthesia is the only way to remove calculus and assess the periodontium. Findings, such as gingivitis, tartar scores, periodontal pockets, ulcers and fractured teeth should be documented on a dental chart. This gives a good pictorial view when discussing the finding with the client to aid their understanding (Figure 11). See the statement from the RCVS on anaesthesia-free dentistry: tinyurl.com/ycw9kxvs
Periodontal disease is a prevalent condition in dogs that can have serious consequences if left untreated.
Early identification and intervention are key to maintaining our patients’ oral health and overall well-being.
Regular brushing and professional veterinary care are essential components of an effective oral health routine.
By recognising the signs of periodontal disease early and taking steps for our clients to manage it at home, you can help your patients lead a healthier, more comfortable life.
Karen Carver is from Dunbar, East Lothian. She attended Telford College and became a registered veterinary nurse in 2011. After time in an Edinburgh hospital, working in a number of roles, including the challenge of a busy out-of-hours emergency clinic, Karen moved to DentalVets, a dentistry referral centre in East Lothian in 2014. She is now leading its nursing team as head veterinary nurse and working her way through the VTS (Dentistry) programme. Karen is passionate about dentistry and aims to inspire fellow veterinary nurses to become more involved in veterinary dentistry, and end the stigma of boring dental procedures.
Ingrid Tundo graduated from Milan University in 2014. She moved to Swindon in 2017 and joined the Eastcott Referrals dentistry team, where she started her full-time residency programme. Ingrid is especially interested in maxillofacial surgery, congenital abnormalities and advanced head imaging. In 2020, she moved to Scotland to start a new position as a senior lecturer at The University of Edinburgh, where she founded the Dentistry and Maxillofacial Surgery Department. Motivated by her passion for maxillofacial surgery, Ingrid joined DentalVets in 2022 as the head of the maxillofacial surgery department. She teaches several national and international dentistry courses.